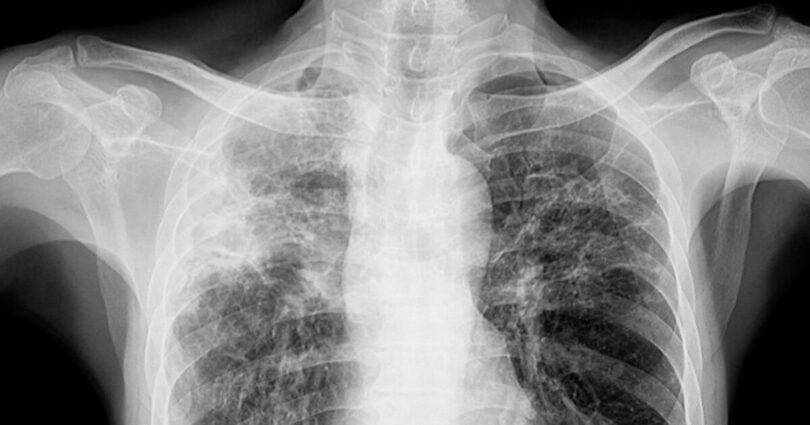
The chest x-ray of a patient with TB in their lungs (Image: Getty)
Many people think of tuberculosis as something out of a Charles Dickens novel. But it seems that TB is no longer an illness of the past. It continues to be one of the world’s most prevalent diseases and has infected Brits as recently as last month. A bacterial infection that spreads through the air, TB usually affects the lungs.
It can also damage other parts of the body, including the brain and spine. Around the world, more than a million people die from TB every year. That’s not because we lack the science to treat it, it’s because too many countries don’t have the funding or health systems to control it properly.
What you need to know
Despite the many advances in public health and sanitation,TB never really disappeared here. Numbers dropped afterthe Second World War, but the disease has always been therein the background. Outbreaks still happen, particularly in large cities. Recently, 10 workers at Amazon’s warehouse in Coventry tested positive for TB. The outbreak is an uncomfortable reminder that dangerous diseases can creep back on to British soil – and we should be prepared for more cases to emerge as we feel the effects of recent cuts to global TB programmes.
In a world of constant travel and movement, diseases travel too. After all, infectious diseases do not respect borders. Around three-quarters of UK TB cases are linked to people who migrated from countries with high levels of TB, and cases among UK-born people are now rising too. This shows how TB in the UK is inextricably linked not only to health and welfare in the country, but also to health and infectious disease programmes overseas. If these programmes aren’t successful, we also feel the consequences.
The trend of TB cases is already off track compared to our aims to oust it in the UK by 2035. And, if TB cases continue to rise, the UK could even lose its “low incidence” status with the World Health Organization, a label that reflects decades of progress. That would be a sobering milestone, and a clear signal complacency has a cost.
Read more: I’m a comedian and I know what it’s like to nearly die on stage
Read more: I’ve seen hundreds of hearts stop – and some people ‘come back from the dead’

Prof Tim Hallett says TB is no longer an illness of the past (Image: Courtesy Timothy Hallett)
How TB spreads
When someone with active TB in their lungs coughs, sneezes, laughs, sings or even talks, they release tiny droplets that can carry the bacteria and it spreads in the air. If other people breathe in those droplets, especially in closed, poorly ventilated spaces, they can become infected.
TB is much more likely to spread in crowded homes, workplaces, hostels or other indoor settings where people spend long periods together. Some people carry TB bacteria in their body without symptoms (known as “latent TB”) and are not contagious. But if the disease becomes active, they can pass it on unless they are diagnosed and treated.
What are the symptoms?
TB symptoms often build up slowly. Common symptoms include a cough that lasts more than three weeks, coughing up blood or phlegm, fever, night sweats, weight loss, tiredness and chest pain. TB can also affect other parts of the body, causing different symptoms depending on where it takes hold.
What treatments are there?
TB can usually be cured. Treatment involves taking a combination of antibiotics for several months. Most people start to feel better quickly, but it’s very important to finish the full course, even if symptoms improve. Stopping early can allow the infection to come back and makes drug-resistant TB more likely. This drug-resistant type is much harder to treat and can take far longer, with more side effects. That’s why stopping TB from spreading, in the UK and around the world, matters so much.
In the UK, early testing, contact tracing and the BCG vaccine (which is over 100 years old and still in primary use all around the world) all help. But the jab only offers partial protection and doesn’t stop the main kind of TB that spreads between adults. That’s why new vaccines in development really matter.

TB can be detected and diagnosed by a blood test (Image: Getty)
Truth and myths about TB
Myth: TB is a disease of the past.
Reality: TB is still widespread globally and continues to affect thousands of people in the UK each year.
Myth: Only homeless people or people in extreme poverty get TB.
Reality: TB can affect anyone. While poverty, overcrowdingand poor access to healthcare increase risk, cases occur acrossall backgrounds.
Myth: TB is easy to cure, so it’s not a big deal any more.
Reality: TB is treatable, but it can take months. Drug-resistant TB is a global threat and is far more difficult and expensive to treat.

Cutting money from global healthcare schemes puts us all at risk (Image: Getty)
How TB can be stopped
Here’s the blunt truth: you can’t separate “TB abroad” from “TB at home” any more. Cutting funding for global health might look like an easy saving, but it’s short-sighted.When TB spreads unchecked in poorer countries because clinics are underfunded and treatment is interrupted, it doesn’t just stay put. People travel, supply chains move, and infections move with them. The knock-on effects show up in British workplaces, GP surgeries and hospitals.
Lives are currently being put at risk following recent aid cuts around the world, including by major donors like the US and the UK, which has put vital programmes in jeopardy. Programmes that the UK helps support through the Global Fund could help reduce by almost half the rate of TB incidence in high-burden countries overseas – reducing TB in Britain and saving the NHS money. When those programmes falter, TB gains ground. And when TB gains ground anywhere, everyone feels the consequences. Investing in global health is not charity: it’s in our own interest. Every pound spent overseas stopping TB – or, for that matter, on improving health and healthcare – saves many more pounds later on here in testing, treatment and outbreak control. Strong health systems abroad mean fewer infections reaching our shores, and fewer outbreaks for Britain to deal with down the line.
Do I need to be worried?
You may be at higher risk of TB if you work in settings where you’re in close contact with lots of people, such as healthcare, social care, shelters, hostels, prisons or crowded workplaces, have a weakened immune system, or are very young or older, as these age groups are more likely to become seriously ill if infected.
The good news is there are simple ways to reduce the risk. If you’re offered TB screening through work or the NHS, take it up. If you’ve been in close contact with someone diagnosed with TB, get checked even if you feel fine – TB can sit quietly before causing symptoms. Good ventilation in crowded indoor spaces helps, as does not ignoring symptoms that linger for weeks. TB is treatable, and early diagnosis protects not just you, but your family, friends and colleagues too.
Source link